Researchers analyzed the genomes and behavioral profiles of 1,300 golden retrievers and found that several behavioral traits—such as trainability, fear of strangers, and aggression toward other dogs—are shaped by specific genetic variants.


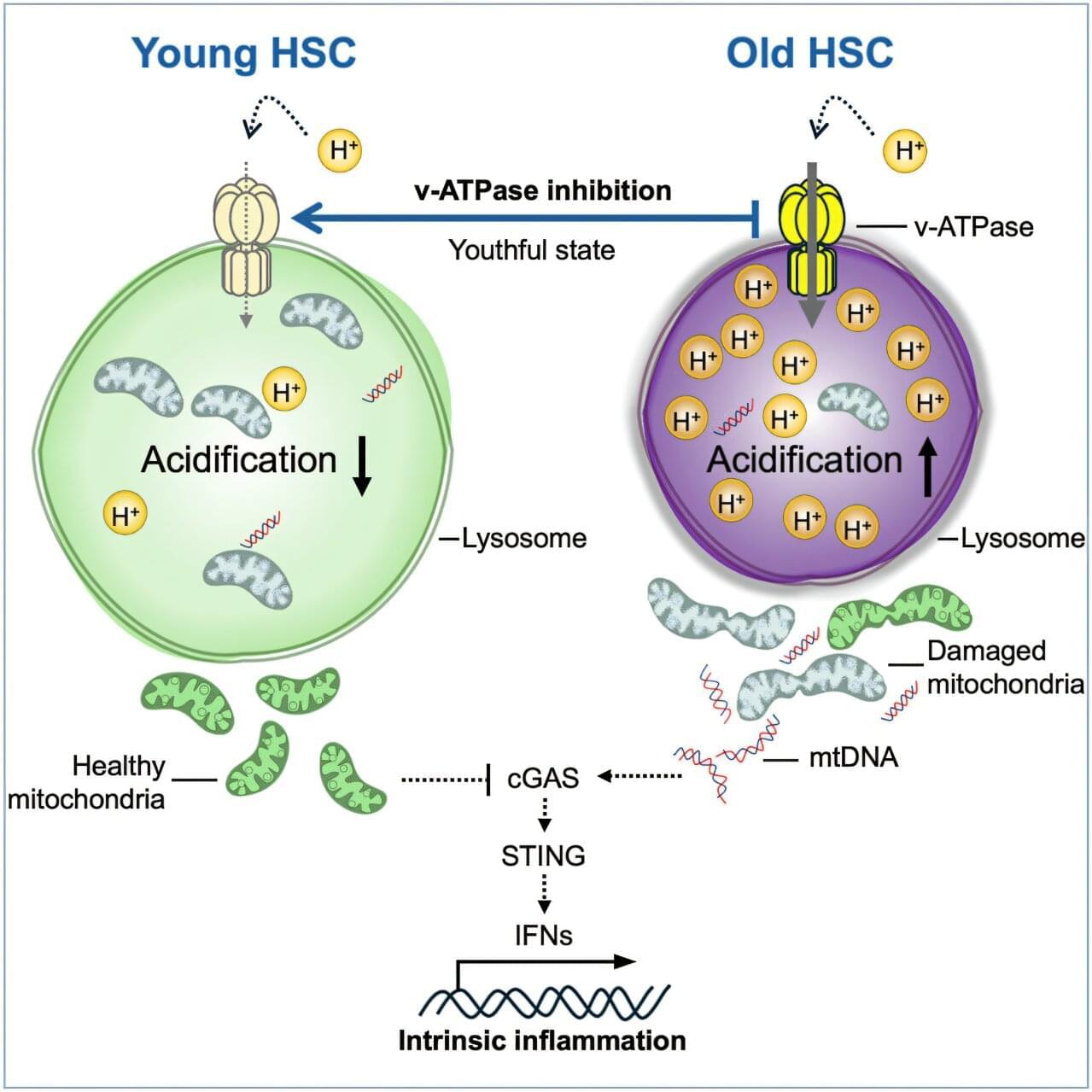
Researchers at the Icahn School of Medicine at Mount Sinai have discovered how to reverse aging in blood-forming stem cells in mice by correcting defects in the stem cell’s lysosomes. The breakthrough, published in Cell Stem Cell, identifies lysosomal hyperactivation and dysfunction as key drivers of stem cell aging and shows that restoring lysosomal slow degradation can revitalize aged stem cells and enhance their regenerative capacity.
Lysosomes are specialized structures that act as the cell’s recycling system, breaking down proteins, nucleic acids, carbohydrates, and lipids. Lysosomes accumulate and degrade waste, and eventually recycle it to be reused in biosynthetic processes. Lysosomes can also store nutrients to be released when needed. Lysosomes are recognized as pivotal for regulating metabolism in the cell, both catabolism (breaking down complex molecules to simple ones) and anabolism (building complex molecules from simpler ones).
The study, led by corresponding author Saghi Ghaffari, MD, Ph.D., Professor of Cell, Developmental, and Regenerative Biology at the Icahn School of Medicine and a member of the Black Family Stem Cell Institute, focuses on hematopoietic stem cells (HSCs). These are the rare long-lived cells in the bone marrow responsible for generating all blood and immune cells.
Researchers have suspected for some time that the link between our gut and brain plays a role in the onset of Parkinson’s disease.
A recent study identified gut microbes likely to be involved and linked them with decreased riboflavin (vitamin B2) and biotin (vitamin B7), suggesting an unexpectedly simple treatment that may help: B vitamins.
“Supplementation therapy targeting riboflavin and biotin holds promise as a potential therapeutic avenue for alleviating Parkinson’s symptoms and slowing disease progression,” said medical researcher Hiroshi Nishiwaki from Nagoya University in Japan, when the paper was published in May 2024.

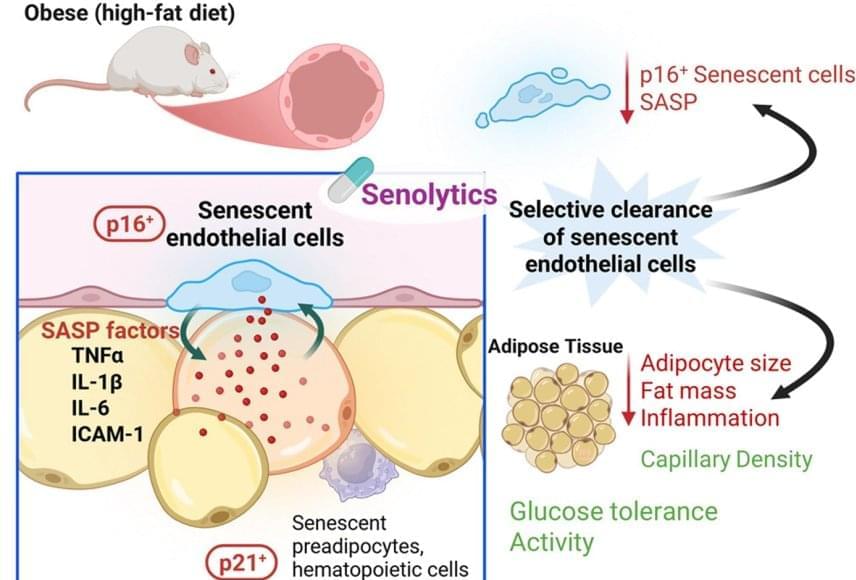
Previous research by the investigators showed that eliminating senescent cells with drugs called senolytics improved metabolic function, the body’s method for turning food and drink into energy.
In the current study, investigators focused on senescent blood vessel cells. They selectively removed these cells from obese laboratory mice and found that the animals’ inflammation and fat mass were reduced—and blood sugar levels improved.
When the investigators transplanted senescent blood vessel cells into lean laboratory mice, those mice developed inflammation in fat tissue and metabolic dysfunction.
The lead said this occurred because senescent blood vessel cells release high levels of inflammatory molecules.
The investigators next treated both groups of mice with fisetin, a naturally occurring senolytic compound, and found that the mice had fewer senescent blood vessel cells and improved diabetic symptoms. Investigators saw a similar decline in senescent blood vessel cells when they treated tissue samples from obese human patients with fisetin.
Investigators found that aged blood vessel cells play a key role in the development of metabolic disorders, including diabetes. The preclinical findings, published in Cell Metabolism, could lead to new treatments for these complex disorders.
A new pill for treating dementia is delivering promising “topline” results in early-stage clinical trials, according to a recent press release by its makers.
The treatment, called VES001 after its developer Vesper Bio, is designed to tackle frontotemporal dementia (FTD) – the most common type of dementia in the under-60s.
In a two-part preliminary safety trial at two medical centres in the Netherlands and the UK, VES001 was given to people showing no signs of FTD, including six volunteers with an increased genetic risk for the condition.
PCE, a dry-cleaning chemical found in many everyday products, has been linked to tripled risk of serious liver damage. Scientists have uncovered a new environmental culprit behind liver disease: tetrachloroethylene (PCE), a chemical used in dry cleaning and household products. The study found that people with PCE exposure were three times more likely to develop severe liver scarring, even when traditional risk factors like alcohol or obesity were absent. The chemical is widespread in air, water, and consumer goods, making it a stealthy threat to public health.
Liver disease most often develops due to one of three major causes: excessive alcohol use, the buildup of fat in the liver associated with obesity, diabetes, and high cholesterol, or viral infections such as hepatitis B and C.
Researchers from Keck Medicine of USC have identified another potential cause of liver damage. A new study published in Liver International links tetrachloroethylene (PCE), a chemical widely used in dry cleaning and found in household products like adhesive glues, spot removers, and stainless steel polish, to serious liver harm.
